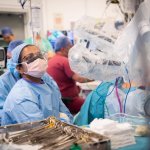
Life during the pandemic has been difficult for most of us. But there’s no doubt some occupational groups have had a particularly tough time, especially NHS workers.
Many NHS staff have dealt with inordinate numbers of critically ill patients. Some have been trying to provide care in a far from ideal situation, knowing that doing so will lead to poor outcomes for their patients. This is having an impact on their mental health.
My recent study of staff working in critical care during the pandemic showed they report more than twice the rate of probable post-traumatic stress disorder (PTSD) found in military veterans who’ve recently experienced combat.
While the situations may be different, there might be some lessons we can learn from studied of PTSD in military veterans to help NHS workers cope during the pandemic.
A solution
Despite the difference in context between the military on deployment and healthcare staff working during the pandemic, there are a few things we can learn. These can be broken down into two parts. Firstly, how to sustain wellbeing while the trauma is ongoing and, secondly, what can be done during “recovery” to optimise mental health outcomes.
We know the best way to protect the mental health of teams who are in the middle of a crisis is to ensure the social bonds between staff are as strong as they can be. This means buddying up staff on shift, encouraging all staff to be alert for indicators of stress and to be supportive and compassionate with each other.
Where possible, implementing a formal peer support system might be helpful. One example of these is called Trauma Risk Management (TRiM), which originated in the military but is now widely used to support the mental health of trauma-exposed personnel across a range of occupations.
There is high quality evidence showing the relationship between staff and their immediate supervisor is critically important. Studies have shown relatively brief training to bolster supervisors’ confidence in having “psychologically savvy conversations” with their teams can lead to up to 90% reduction in sickness absence.
There’s also some evidence that enabling staff to reflect on their experience can help, by developing a meaningful narrative which focuses on all the team being “in it together” and doing the best they can. This can prevent moral injury – psychological distress caused by actions which violate your moral or ethical code – and the associated poor health.

Gorodenkoff/Shutterstock.com
PTSD in NHS staff
Changing your mindset from saving lives in arduous circumstances, with the threat of personal infection, to discussing dinosaurs with a young child or the price of pasta with your partner, and then back, may be rather challenging.
While most healthcare workers will be used to dealing with illness and death, the duration and severity of working during a pandemic and exposure to trauma has been shown to correlate well with potential psychological impact. And of course while soldiers on deployment know the date they’ll return to a safe and reassuring environment; this isn’t the case for healthcare workers at the moment. No one really knows when, or indeed if, the pandemic will end.
Most studies of groups exposed to traumatic events measure the presence or absence of PTSD once the traumatic event is over. These studies have examined military personnel or disaster workers who’ve returned from deployment, or emergency services staff after they’ve attended a major incident.
Measuring mental health symptoms once a crisis has ended is very different to doing so during an ongoing crisis, when a degree of distress, fear or even excitement would be expected. Unlike personnel who deploy away from home to a war or disaster zone for a discrete period of time, critical care staff have to cope with regularly transitioning between intensely challenging workplaces and their usual domestic environment.
Long term
In the longer term it will be necessary to actively monitor staff, which is the recommendation of the National Institute for Health and Care Excellence (NICE) for the initial management of traumatic stress reactions. This can be done by alert, sensitive and compassionate managers and may be helped by providing staff, and indeed their families, with information about what to look out for.
It’s important that staff who do unfortunately develop mental health problems get timely access to NICE recommended treatments and that all care provision has a specific “return to work” focus. Being at work, where possible, is good for the NHS and the staff member themselves.
The pandemic is a tough time for everyone, in particular NHS staff. But there’s good reason to think with the right ongoing support, and the use of evidence-based approaches during recovery, this burden of ill health can be reduced as long as we take this seriously and plan for the time ahead.
![]()
Neil Greenberg works as part of March on Stress which is a psychological health consultancy that provides some support for healthcare staff. He receives funding from NIHR for healthcare related research work. He is affiliated with the Royal College of Psychiatrists.