algae/Shutterstock
People who have been seriously unwell and treated on intensive care units can expect to take some months to recover fully, regardless of their ailment. However, with COVID-19, evidence is mounting that some people who have had relatively mild symptoms at home may also have a prolonged illness. Overwhelming fatigue, palpitations, muscle aches, pins and needles and many more symptoms are being reported as after-effects of the virus. Around 10% of the 3.9 million people contributing to the COVID Symptom Study app have effects lasting more than four weeks.
Chronic fatigue – classified as fatigue lasting more than six weeks – is recognised in many different clinical settings, from cancer treatment to inflammatory arthritis. It can be disabling. If 1% of the 290,000 or so people who have had COVID-19 in the UK remain under the weather at three months, this will mean thousands of people are unable to return to work. They will probably have complex needs that the NHS is ill-prepared to address at present.
COVID-19 is not the only cause of chronic fatigue. Prolonged fatigue is well recognised after other viral infections such as the Epstein-Barr virus, which causes infectious mononucleosis (also known as glandular fever). Post-viral fatigue was also seen in a quarter of those infected with the original Sars virus in Hong Kong in 2003.
When it comes to treating chronic fatigue, the emphasis previously has been on effective treatment of the underlying disease, in the belief that this would diminish the fatigue. However, for most viral infections there is no specific treatment, and because COVID-19 is so new, we don’t yet know how to manage post-COVID fatigue.
What might be causing post-COVID fatigue?
Although we know that lasting fatigue can sometimes follow other viral infections, detailed mechanistic insight is, for the most part, lacking. An ongoing viral infection in lung, brain, fat or other tissue may be one mechanism. A prolonged and inappropriate immune response after the infection has been cleared might be another.
However, a previous study has given us some insight. When a chemical called interferon-alpha was given to people as a treatment for hepatitis C, it generated a flu-like illness in many patients and post-viral fatigue in a few. Researchers have studied this “artificial infection response” as a model of chronic fatigue. They found that baseline levels of two molecules in the body that promote inflammation – interleukin-6 and interleukin-10 – predicted people’s subsequent development of chronic fatigue.
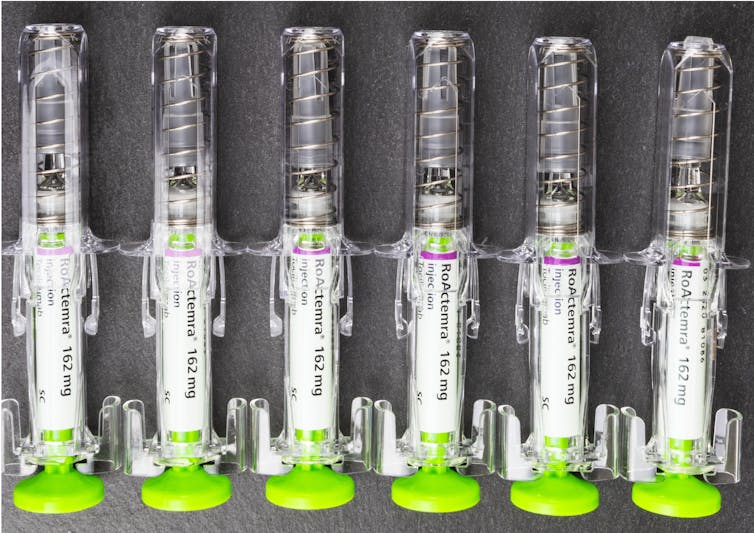
Of particular interest, these same pro-inflammatory molecules are seen in the “cytokine storm” of severely ill COVID-19 patients. This suggests there might be a pattern of immune system activation during the viral infection that is relevant to ongoing symptoms. Further support for interleukin-6 playing some sort of role comes from the successful use of tocilizumab – a treatment that lessens the impact of interleukin-6 and reduces inflammation – to treat severe COVID-19.
Wirestock Images/Shutterstock
What needs to happen next
At TwinsUK at King’s College London, we investigate the genetic and environmental factors that influence disease by studying twins. We’re using the COVID Symptom Study app to examine the long-lasting symptoms being reported. We’re sending out questionnaires to the volunteer adult twins on our database, many of whom were included previously in immune system studies long before the coronavirus epidemic. We aim to define “post-COVID syndrome” and look at markers in the blood to shed more light on the immune mechanisms contributing to long-term symptoms.
This will be a challenging study to design: people with COVID-19 have had more than just a viral infection in the normal run of things. Their illness has taken place during unprecedented social change, restriction in movement, and a time of great anxiety and difficult-to-quantify risks – all accompanied by 24-hour rolling news. Some patients have been very sick at home and thought themselves close to death. For this reason, we’ll also be examining post-traumatic stress, as the interpretation of reported symptoms must be set in context.
Chronic fatigue doesn’t lie within the remit of a single medical speciality, so it’s often overlooked on medical school curricula, and doctors are poorly trained in the diagnosis and management of chronic fatigue. But recent progress has been made and online training is available for doctors that covers how to care for at least those with the most severe symptoms.
Guidance for patients in managing chronic fatigue and how to conserve energy is also now available. The important thing to stress is that taking out a gym membership and pushing exercise is the wrong thing to do and can set people back considerably. Small efforts – mental or physical – should be followed by rest. Return to work, when it happens, should be a gradual and graded process. Learning to pace activities is very much the order of the day.
![]()
Frances Williams receives funding from Versus Arthritis and the Kennedy Trust to perform studies of post-COVID symptoms.











