An individual’s genetic makeup could influence the effectiveness of weight-loss injections, a new study suggests.
Researchers discovered that specific gene variants can predict both the degree of weight loss achieved and an individual’s likelihood of experiencing side effects like nausea and vomiting.
This insight could partially explain why some people lose weight faster than others on these medications, while others are more vulnerable to adverse reactions.
Published in the journal Nature, the findings offer a pathway towards developing precision medicine, allowing doctors to tailor treatments based on genetic profiles.
The new study examined data from almost 28,000 people registered to the genetics website 23andMe and self-reported data on their use of GLP-1 receptor agonist weight-loss treatments including semaglutide, such as Wegovy, and tirzepatide, also known as Mounjaro.
Using genetic data, researchers found that variations in two genes involved with hormones in the gut, which regulate appetite and digestion, could play a role in how these drugs work.
One, the GLP1 receptor variant rs10305420, was associated with a slightly greater decrease in body mass index (BMI) among people taking GLP-1 drugs.
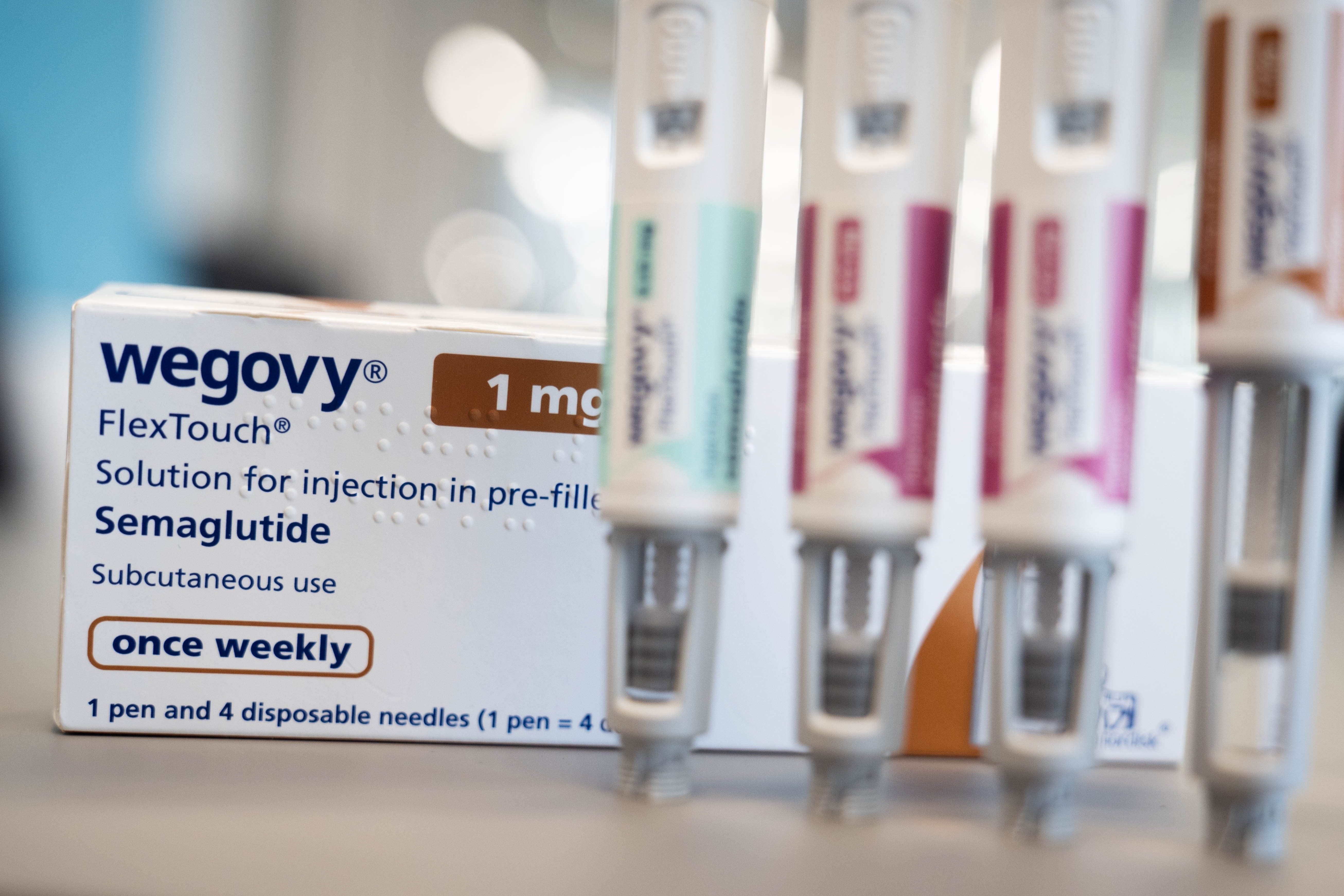
Another, rs1800437 in the gastric inhibitory polypeptide receptor gene, was linked with side effects of nausea and vomiting in people taking tirzepatide, but was not associated with how much weight they lost.
The researchers, led by experts from 23andMe and The University of Copenhagen, said that these genetic differences may partially account for differences in weight loss.
Though other non-genetic factors play a role, including gender, age and which treatment a person takes.
“Our study detected a robust genetic association with GLP-1 medication weight loss efficacy and associated side effects,” the authors wrote.
But they stressed that the effect was “modest” as they called for future studies to explore the role of genetics in these treatments further.
Commenting on the paper, Dr Marie Spreckley, research programme manager at the University of Cambridge, said the study “provides biologically plausible evidence that variation in the drug target itself (GLP1R) and related pathways (GIPR) contributes to inter-individual variability in response.
“However, the magnitude of these genetic effects is small in clinical terms.
“Importantly, non-genetic factors such as sex, drug type, dose, and duration appear to explain a substantially larger proportion of variability.”
Dr Spreckley added: “In terms of how this fits with the wider evidence, it reinforces that while there is substantial variability in response to GLP-1 therapies, genetics is only one part of a much more complex picture.
“Behavioural, clinical, and treatment-related factors remain the dominant drivers of outcomes.
“Overall, this is an important step towards understanding variability and the potential for future precision approaches, but the effects are modest and the evidence is not yet sufficient to support using genetic information to guide treatment decisions in routine clinical practice.”