Prostock-studio/Shutterstock
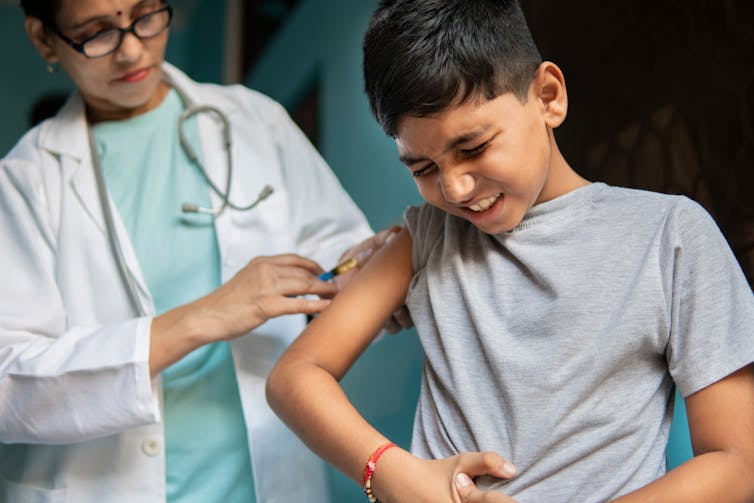
Every individual’s experience of pain is unique – but that makes it harder to treat. The experience of pain remains impenetrable to scientists because it is so variable. So researchers and clinicians still rely on subjective ratings, such as asking patients to rate their pain on a scale of zero to ten.
But my recent work, in collaboration with my colleague Enrico Schulz and his team, showed new insights into a type of brainwave called gamma oscillations that scientists think may be linked to pain perception.
For the first time, we showed that gamma oscillations differ greatly between people, but that people’s response pattern to pain stayed the same over time. In other words, people who show no waves when in pain will probably not show them in a subsequent recording (when experiencing pain again), whereas those who show a large response will probably show it again.
Pain is variable by definition: the International Association for the Study of Pain defines it as a personal, unpleasant sensory and emotional experience that is influenced by biological, psychological and social factors.
Pain is often different in quality (dull, sharp, shocking, throbbing) and it may be hard to remember properly. To complicate matters, although nociception (the unconscious processing of unpleasant stimuli) usually leads to pain, research shows that one can exist without the other.
An objective marker of pain would bypass the distortions caused by cognitive and social factors. And it would help patients who cannot communicate (such as those in a vegetative state) as well as young children and babies.
The long search for a pain gauge
Over the past few decades, technological advancements gave researchers the opportunity to finally start developing an objective measurement of pain.
In the early 1990s, neuroimaging techniques such as PET scans and fMRIs became a popular way to study pain. This led to a focus on physiological measures of brain activity.
Scientists became excited by the idea of identifying some sort of “pain centre” or “pain network” within the brain. However, studies of the brain activation during pain experiments showed that even innocuous stimuli (for example, warmth, touch or vibration when participants weren’t expecting it) can activate the brain similarly to painful stimuli.
Studies have also shown that the brain’s response to painful heat is strongly influenced by the person’s level of alertness and attention. Both your brain response and your conscious perception of pain are influenced by how much attention you pay to it.
Clovera/Shutterstock
There is growing evidence that brain response to pain doesn’t always have a meaningful relationship to the level of pain a person is experiencing – heightened brain activity doesn’t always mean heightened pain. Contextual factors, study methodology and biological differences between people can all affect brain activity.
So, it became clear that technology alone wouldn’t give us an objective measure of pain. Researchers needed to understand more about the brain’s response to stimulation.
Brain oscillations
Decades of research have shown the type of brainwave called gamma oscillations are a good measure of human response to stimulus in general, not just pain. In the 2000s, experimental work showed that gamma oscillations increased in amplitude following both brief and prolonged thermal painful stimuli in healthy volunteers.
Gamma oscillations may control the connectivity between different brain regions. Patient research and recording of electrical activity within the brain seemed to support the idea that gamma oscillations could reflect pain perception better than any other brain response to pain.
Our recent work has demonstrated how gamma waves synchronised with painful thermal stimulation are unique to each person. For our experiment, we briefly induced pain using a thermal laser in 22 healthy male volunteers in their 20s and 30s, then recorded their gamma wave responses. This not only pinpointed the extreme variability in people’s gamma waves, but also showed that a person’s response pattern is stable across time.
Our analysis of a separate study published in 2021, independent from ours but using similar methodology, also demonstrated variability between participants in their gamma wave response.
What our results mean
The more we understand about people’s unique response to pain, the closer we can get to giving them the right pain relief.
Our findings suggest we must rethink our interpretation of the relationship between pain and gamma oscillations, but that it’s still too early for general rules. Some people will feel pain and have no gamma response, while others will show a large response.
It is also important to remember that brain mechanisms triggered by experimental pain in young healthy people are not necessarily the same as those who have been shaped by long-term pain experience. For example, people with chronic pain conditions may have changes in their brain structure and response to pain.
As yet, no clinical trials involving gamma waves have been carried out, perhaps due to technical and ethical challenges involved in experiments that study chronic pain patients.
So, we don’t yet know why different people have such different gamma wave responses to pain. But if gamma waves can reliably predict pain in a substantial percentage of the population, we could use this to diagnose, manage and treat pain conditions.
![]()
Elia Valentini does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.











